As a recap of the previous articles, we learned that liver disease has many types. Fatty liver disease is a condition where fats build up in the liver (and it makes up more than 5-10% of your liver’s weight).
There are two main types of this disease: Alcoholic Fatty Liver Disease which is caused by excessive alcohol intake and Non Alcoholic Fatty Liver Disease (NAFLD), a condition in which fat builds up in the liver but is not related to alcohol use. It tends to develop in people with obesity, diabetes, high cholesterol or high triglyceride (fat) levels in their blood. It is prevalent among 30-40% of American adults.
As part of the observance of Liver Month, we will focus on the nutritional aspects in the prevention and management of fatty liver diseases.
Alcoholic Fatty Liver Disease
From the word itself, it is caused by alcohol. A sensible preventive measure is to avoid drinking alcohol or if you already are drinking it, do so in moderation; avoid heavy drinking.
“Moderate alcohol consumption is defined as having up to 1 drink per day for women and up to 2 drinks per day for men. This definition refers to the amount consumed on any single day and is not intended as an average over several days. [1]
Heavy drinking among men is usually defined as 15 drinks or more per week while among women it is 8 drinks or more per week.
Patients diagnosed with alcohol related fatty liver disease are usually nutritionally evaluated. Many patients are lacking in nutrients needed by the body (malnourished) due to poor appetite, unhealthy diet, malabsorption (because of the ineffectiveness of the liver) and empty calories (alcohol has “empty” calories, it gives 9 kcal/gram but without any nutrient like vitamins, minerals, etc. and it requires lots of energy to be processed in the body) [2]. Many hospitalized patients are initially given high energy and high protein diet with vitamin and mineral supplements.
Alcoholic fatty liver disease patients are advised to stop drinking alcohol and eat a well-balanced diet. They need to work together with their doctor and dietitian/nutritionist to work out a diet plan, as well as nutritional supplements tailored to their case.
Non-alcoholic Fatty Liver Disease (NAFLD)
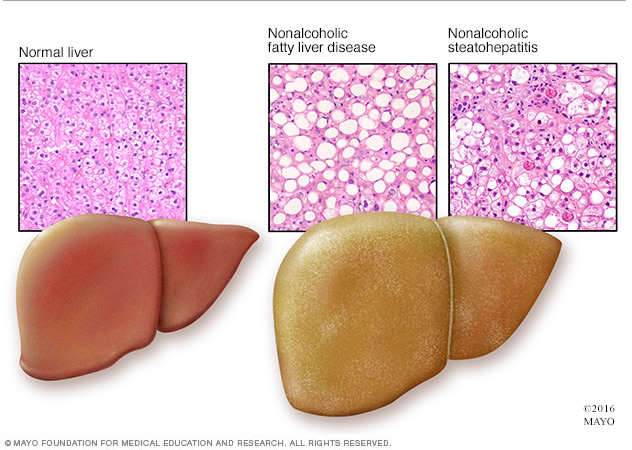
It is the build-up of fats in the liver which is not due to alcohol. NAFLD is often linked to obesity, diabetes, high cholesterol or fats in blood and metabolic syndrome (presence of any three of the following: high levels of triglycerides in the blood, low levels of HDL cholesterol in the blood, high blood pressure, higher than normal blood glucose levels, large waist size). It can progress into non-alcoholic steatohepatitis (NASH) where there is inflammation and liver cell damage eventually leading to liver cancer.
Prevention strategy for NAFLD includes eating a well-balanced and healthy diet, maintaining or achieving a healthy body weight, performing healthy lifestyle like regular physical activity, avoiding or stopping alcohol consumption.
Patients diagnosed with NAFLD who are obese or overweight are advised to slowly lose weight, around 7-10% of the initial body weight in a course of 1 year.
Intake of fats is also limited as 1 gram of fat provides 9 kcal/gram (carbohydrate and protein provide 4 kcal/gram). Patients are also instructed to use or consume healthier types of fat (monounsaturated and polyunsaturated fats) than saturated and trans fat.
What are the types & sources of dietary fats?
- Monounsaturated fats – richly found in peanut, olive and canola oils and avocado.
- Polyunsaturated fats – found in nuts like walnut, seeds like flaxseed; plant-based oils; fishes like salmon.
Two types of essential polyunsaturated fatty acids- Omega 3 fatty acids – reduce inflammation and may help lower risk of chronic diseases such as heart disease, cancer, and arthritis. Found in fish, such as salmon and tuna; seafood including algae and krill, some plants, and nut oils [3].They are also found in fish oil supplements.
- Omega 6 fatty acids – along with omega-3 fatty acids, they play a vital role in brain function, and normal growth and development. Omega-6 fatty acids help regulate metabolism, stimulate skin and hair growth, maintain bone health and maintain the reproductive system. The average diet supplies sufficient amount of this fatty acid so supplementation is not recommended unless prescribed by a physician [4]. Food sources include corn, soybean and sunflower oils.

- Saturated fats – found in poultry skin, pork, beef fat, butter, lard, shortening, and all milk and dairy products except fat-free versions [5]. Plant-based oils like palm oil, palm kernel oil and coconut oil. A diet rich in saturated fats can increase total cholesterol in the blood, increase “bad” (LDL) cholesterol, which can lead to obstructions in blood vessels of the heart and elsewhere in the body [6].
- Trans fats – Eating trans fats increases your risk of developing stroke and heart disease. It is also associated with a higher risk of developing type 2 diabetes. Found in fried foods like doughnuts, and baked goods including cakes, pie crusts, biscuits, frozen pizza, cookies, crackers, and stick margarines and other spreads; as well as products with hydrogenated or partially hydrogenated oil in the ingredient list [7].
Other dietary changes prescribed by the physician include:
-
- Eating foods with low glycemic index [8] (foods with low glycemic index, e.g. oats, chickpeas, lentils, wholegrain, mushrooms, leafy greens, are more gradually digested and absorbed by the body thus cause a lower and slower rise in blood glucose and insulin levels).
- Avoidance of food and drinks with high amounts of simple sugars, especially fructose. Avoid candy, regular soda, sweetened beverages and other foods/drinks with added sugars including high-fructose corn syrup. Choose naturally sweet foods (e.g. fruit) if you want some sweetness in your diet [9].

Processing of fructose in the liver not only leads to fat build up but also to the following [10]:
-
- Elevates triglycerides
- Increases harmful LDL (so-called bad cholesterol)
- Promotes the build-up of fat around organs (visceral fat)
- Increases blood pressure
- Makes tissues insulin-resistant, a precursor to diabetes
- Increases the production of free radicals, energetic compounds that can damage DNA and cells.
Other nutrition-related approaches:
Aside from the items listed found to be beneficial to NAFLD (wolfberry/ goji berry, garlic-derived compounds, red grape–derived resveratrol, and milk thistle–derived substances, coffee, probiotics) in the previous article, the following have also been found to benefit fatty liver diseases:
- Silymarin (richly found in milk thistle) plus vitamin E and low calorie diet improved test results of patients [11].
- DHA (an omega-3 fatty acid) plus vitamin D treatment improved insulin-resistance, lipid profile and liver function tests [12].
- Treatment with taurine combined with tea polyphenols could relieve NASH [13].
- A study [14] on natural antioxidants like anthocyanins (found in red orange juice, raw red raspberry), catechins (in green tea infusion), resveratrol (500-600 mg per day, in black grapes), silymarin (from dried milk thistle fruit) are found to have beneficial effects in NAFLD patients.

Don’t forget the benefits of physical activity combined with dietary intervention on the prevention and management of fatty liver disease.
Conclusion
No matter what health condition you are in right now, always take care of your liver. It serves a lot of functions in our body. Nutrition, Healthy diet, exercise and lifestyle practices go hand-in-hand and are major keys to prevent and treat fatty liver diseases.
Discover the surprising reason many people experience fatigue, weight gain, and brain fog — and how supporting your liver may help improve your overall health.Watch the full presentation here.
References
- Centers for Disease Control and Prevention. (2017). Alcohol and Public Health. Retrieved from https://www.cdc.gov/alcohol/faqs.htm
- British Liver Trust. (n.d.). Dietary Advice For Specific Liver Conditions. Retrieved from https://www.britishlivertrust.org.uk/liver-information/diet-and-liver-disease/dietary-advice-for-specific-liver-conditions/
- University of Maryland Medical Center. (2017). Omega-3 fatty acids. Retrieved from http://www.umm.edu/health/medical/altmed/supplement/omega3-fatty-acids
- University of Maryland Medical Center. (2017). Omega-6 fatty acids. Retrieved from http://www.umm.edu/health/medical/altmed/supplement/omega6-fatty-acids
- National Institute of Diabetes and Digestive and Kidney Disease. (2016). Eating, Diet, & Nutrition for NAFLD & NASH. Retrieved from https://www.niddk.nih.gov/health-information/liver-disease/nafld-nash/eating-diet-nutrition
- American Heart Association, Inc. (2017). Trans fat. Retrieved from https://healthyforgood.heart.org/Eat-smart/Articles/Trans-Fat
- Harvard University. (2015). The truth about fats: the good, the bad, and the in-between. Retrieved from https://www.health.harvard.edu/staying-healthy/the-truth-about-fats-bad-and-good
- National Institute of Diabetes and Digestive and Kidney Disease. (2016). Eating, Diet, & Nutrition for NAFLD & NASH. Retrieved from https://www.niddk.nih.gov/health-information/liver-disease/nafld-nash/eating-diet-nutrition
- WebMD. 2016. How to Eat Right With Fatty Liver Disease. https://www.webmd.com/hepatitis/fatty-liver-disease-diet#1
- Harvard Health Publishing. (2011). Abundance of fructose not good for the liver, heart. Retrieved from https://www.health.harvard.edu/heart-health/abundance-of-fructose-not-good-for-the-liver-heart
- Aller, R., Izaola, O., Gómez, S., Tafur, C., González, G., Berroa, E., Mora, N., González, J.M. & de Luis, D.A. (2015). Effect of silymarin plus vitamin E in patients with non-alcoholic fatty liver disease. A randomized clinical pilot study. European Review for Medical and Pharmacological Sciences, 19(16):3118-24. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/26367736
- Della Corte, C., et. al. (2016). Docosahexanoic Acid Plus Vitamin D Treatment Improves Features of NAFLD in Children with Serum Vitamin D Deficiency: Results from a Single Centre Trial. PLoS One, 11(12):e0168216. DOI: 10.1371/journal.pone.0168216
- Zhu, W., Chen, S., Chen , R., Peng, Z., Wan, J., Wu, B. (2017). Taurine and tea polyphenols combination ameliorate nonalcoholic steatohepatitis in rats. BMC Complementary and Alternative Medicine, 17(1):455. DOI: 10.1186/s12906-017-1961-3.
- Salomone, F., Godos, J. & Zelber-Sagi, S. (2015). Natural antioxidants for non-alcoholic fatty liver disease: molecular targets and clinical perspectives, 36 (1):5-20




